Health Doesn’t Need More Advice. It Needs Better Feedback Loops.
You may also like :
Why data + outcomes change patient behavior, and why they change the economics of care, too.
Written by David Pachkofsky, Founder & CEO Dapper
Estimated read time: 8–10 minutes
Disclaimer: This is educational content, not medical advice. If you’re considering any health intervention, consult a licensed clinician.
The quiet reason most “health plans” fail
Imagine if your bank balance updated once a year.
You’d still have goals. You’d still have motivation. You’d still want to be responsible.
But you’d be operating blind, so small mistakes would compound, and progress would feel abstract.
That’s remarkably close to how healthcare works for many people today. We get:
- episodic visits
- fragmented data (labs in one portal, prescriptions in another, coaching somewhere else)
- delayed feedback
- and unclear “what worked” vs “what didn’t”
Even the National Academies has used this contrast to highlight how far healthcare lags other sectors: banks update records “in real time” while healthcare struggles to continuously learn from the care experience.
When people can’t see cause-and-effect, adherence drops, motivation fades, and the whole “do the right thing” narrative becomes an exercise in willpower.
And willpower is a terrible strategy.
The adherence problem is not a moral failing, it’s a system design problem
The World Health Organization has long pointed out that adherence to long‑term therapies averages only 50% in developed countries, and it’s even lower in many settings.
That single statistic should change how we interpret “patient behavior”:
- People aren’t refusing care because they’re irrational.
- They’re dropping off because the system doesn’t provide the feedback, reinforcement, and continuity needed for long-term follow‑through.
And the downstream costs are immense. One major U.S. analysis estimated the annual burden of suboptimal medication use at >$500B, including avoidable hospitalizations and other avoidable utilization.
This is where “data + outcomes” becomes more than a product feature. If you can close the feedback loop, you can improve adherence, and when adherence improves, outcomes improve, and the economics change.
Why data changes behavior: the psychology of “visible cause and effect”
Behavior change science is consistent on this: self‑monitoring and feedback are among the most powerful levers available.
A 2024 systematic review of feedback in physical activity interventions found that interventions with feedback were more effective than those without feedback (effect size around d = 0.29).
That effect size is not a miracle. It’s not “biohacking.” It’s basic human cognition:
1) Feedback makes progress legible
If you can’t tell whether something is working, you won’t keep doing it. Data turns vague effort into visible progress.
2) Feedback creates reinforcement
Small wins matter. A system that continuously shows “this is moving the needle” reinforces the behavior and makes it more sticky.
3) Feedback converts guessing into iteration
Without data, people run random experiments. With data, they can run informed experiments.
4) Feedback increases perceived control
People will tolerate effort when they feel agency. Outcomes dashboards increase agency.
The evidence in the real world: measurement changes outcomes
This isn’t theoretical. We’ve seen it repeatedly in high‑signal areas where measurement is continuous, not annual.
Wearables: more movement, modest weight impact, measurable cardiometabolic signals
An umbrella review in The Lancet Digital Health reported that wearable activity tracker interventions resulted on average in:
- 1,800 more steps/day
- 40 more minutes/day of walking
- modest but meaningful improvements in weight (about 1 kg reduction) and BMI (about 0.5 kg/m²) in meta-analyses of weight-loss outcomes
These are not trivial. They’re the type of incremental, sustained shifts that accumulate into long-term healthspan gains, especially when they’re durable and paired with coaching, clinical context, and ongoing adjustments.
Continuous glucose monitoring (CGM): tighter control because the feedback is immediate
A systematic review and meta-analysis of randomized controlled trials in type 2 diabetes found CGM use produced a modest but statistically significant HbA1c reduction (0.32%) versus fingerstick self-monitoring.
The key is not the device itself. It’s the behavioral mechanism:
- you eat → you see the response
- you sleep poorly → you see the response
- you exercise → you see the response
The intervention becomes a closed loop, not an abstract recommendation.
Remote patient monitoring: scaling the feedback loop beyond the clinic
Remote patient monitoring (RPM) has expanded rapidly, one U.S. federal review noted that Medicare RPM enrollees in 2022 were more than 10x higher than in 2019.
And the evidence base continues to grow. For example, a 2024 systematic review of RPM interventions (focused on the hospital-to-home transition) synthesized evidence across dozens of studies (mostly RCTs), assessing safety, adherence, quality of life, and cost-related outcomes.
Other digital monitoring approaches show signals on utilization and mortality as well; one focused review referenced within a 2024 digital medicine synthesis reported a mean reduction in hospitalization and mortality in certain monitoring contexts, useful directional evidence, but also a reminder that effects vary meaningfully by condition and intervention design.
Data alone doesn’t change behavior. The loop does.
There’s a trap in digital health: collecting data and calling it “insight.”
But behavior changes when the system delivers five things, reliably:
A practical framework: The Outcomes Loop
- Measurement Biomarkers, symptoms, adherence signals, wearable telemetry, diagnostic
- Interpretation Translating raw numbers into context: What matters? What’s noise? What’s next?
- Action A concrete plan that is easy to execute (meds, lifestyle, supplements, protocols, scheduling)
- Follow‑through Automation, reminders, refill workflows, friction reduction, check-ins
- Adjustment Iterate based on outcomes, like a tuning loop, not a one-time prescriptionIf any one of these breaks, the experience reverts back to “episodic care,” and drop-off becomes the default.
Why outcomes change the economics, not just the health metrics
Once you see healthcare as a feedback-loop problem, the business implications become straightforward.
1) Better outcomes reduce “value skepticism”
In cash-pay markets especially, patients constantly ask: Is this worth it?
2) Adherence improves unit economics (in any model)
When adherence rises, you typically see:
- fewer avoidable acute events
- fewer wasted prescriptions
- fewer “start-stop” cycles
- more predictable utilization
Societal economics on the overall burden of suboptimal medication use in the U.S are huge (more than $500B per year by some estimates).
3) Longitudinal data becomes a compounding asset
The more patients stay engaged, the more longitudinal data you generate. That enables:
- better personalization
- better protocol refinement
- better risk stratification
- stronger clinician decision support
This is the backbone of a “learning health system”, a system where data from care delivery is continuously analyzed and fed back to improve future care.
4) The system becomes “sticky” because it becomes useful
People don’t stick with apps because they’re pretty.
They stick because the app becomes the place where “my health makes sense.”
That “sense making” is retention.
The overlooked failure mode in many modern health experiences: fragmentation after the prescription
A lot of modern care, especially in functional health and longevity, gets the first part right:
- compelling education
- initial diagnostics
- a prescription or protocol
But then it fractures:
- labs happen elsewhere
- refills are manual
- side effects are unmanaged
- patient questions bounce between inboxes
- supplements and supportive products are disconnected
- outcomes are not tracked in a coherent dashboard
And once the loop breaks, adherence falls back to the global baseline: 50% for long-term therapies.
In other words:
The most important moment is not the prescription.
It’s the weeks and months after the prescription.
That’s where behavior either becomes a habit, or dissolves into drift.
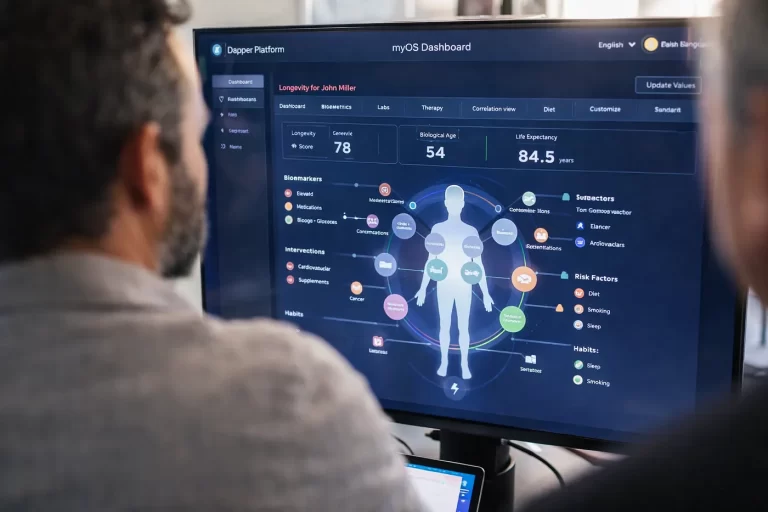
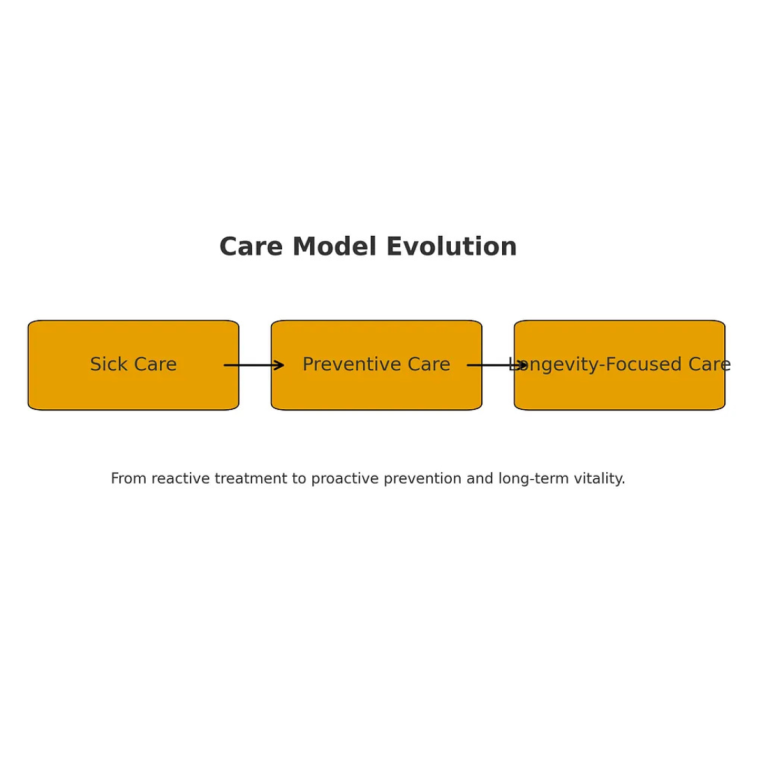
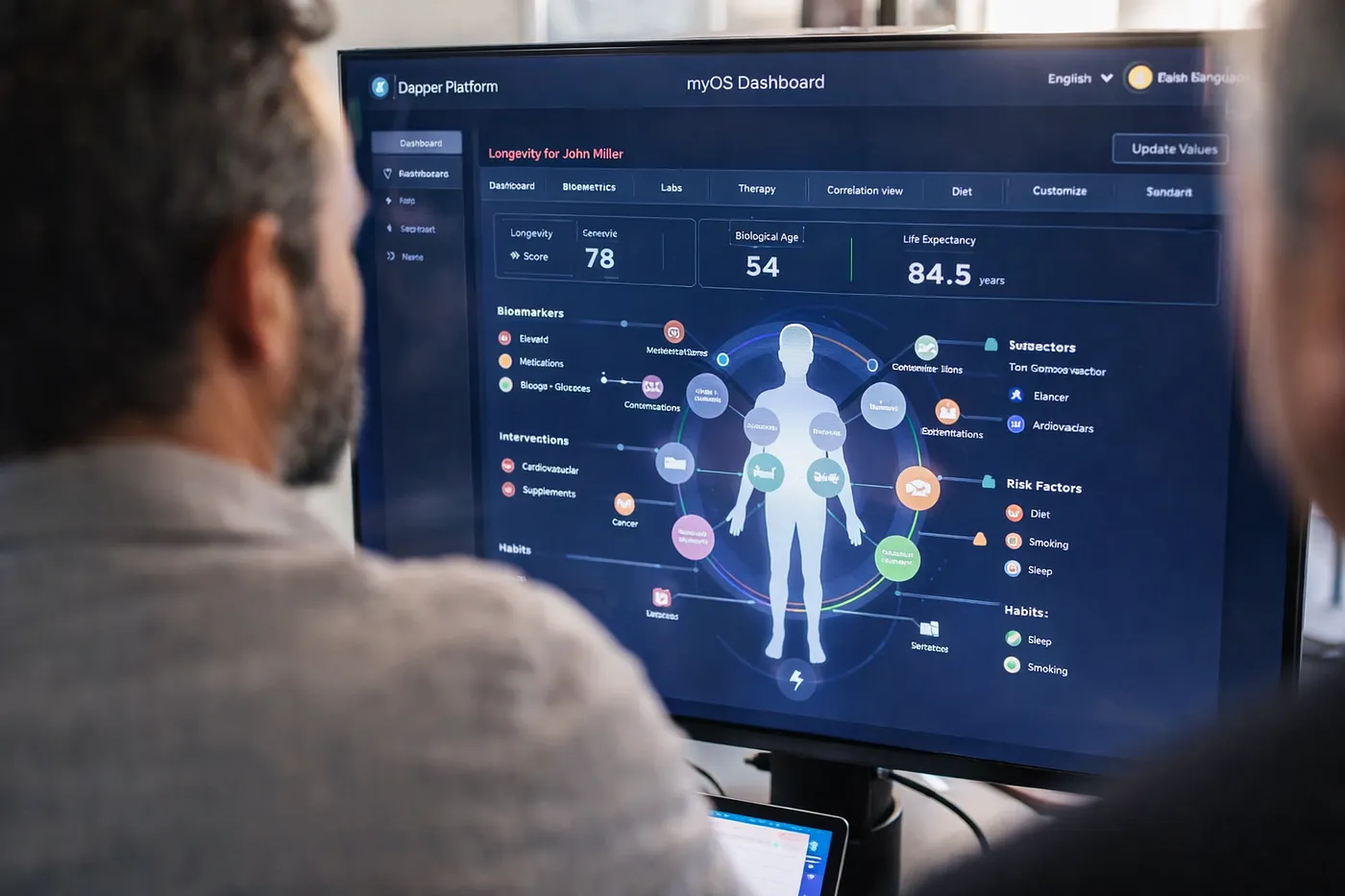
What this means for longevity: data turns “healthspan” into a measurable objective
Longevity care often gets caricatured as expensive optimization. But the deeper idea is simple:
- If you can continuously measure what matters,
- and iteratively adjust interventions,
- you can move from reactive “sick care” to proactive “healthspan management.”
Not by promising immortality.
By building a system where progress is visible and actionable.
The wearables evidence and CGM evidence aren’t “longevity” per se, but they demonstrate the principle:
When people can see cause-and-effect, they behave differently.
Why this matters: the health-span gap is the real problem
Research across 183 WHO member states estimates that the average person spends 9.6 years living in less than full health — and the U.S. has the largest gap at 12.4 years. The same analysis found women experience a meaningfully wider gap than men, driven largely by the burden of chronic disease. In the U.S., the CDC reports that three in four adults have at least one chronic condition, and over half have two or more — making “extended healthspan” not a niche aspiration, but one of the most urgent problems in modern life.
Putting the outcomes loop into practice: the missing “OS” layer
A lot of modern functional health and longevity platforms are impressive at the front end: onboarding, education, diagnostics, and even a strong first protocol.
Where many experiences still break down is after the prescription.
That’s where care often becomes fragmented again — labs live in one place, refills in another, side effects get handled inconsistently, supplements are disconnected, progress tracking is sporadic, and patients are left to stitch together what’s working and what isn’t.
But if outcomes are the goal, the post‑prescription phase is the main event.
A real “health operating system” has to keep the outcomes loop intact end‑to‑end:
- Measure (labs + continuous signals)
- Interpret (what matters, what changed, what’s next)
- Act (a plan that is easy to execute)
- Follow through (automation, adherence, continuity)
- Adjust (iterate based on outcomes, not guesswork)
Disclosure: I’m building a platform in this space (Dapper). Our internal term for the end state is myOS — a physician-led operating system for longevity care. The key idea isn’t “more features.” It’s closing the loop so outcomes don’t fall apart after the prescription — because that’s where behavior either becomes a habit or dissolves into drift.
Closing thought: the next era of healthcare will be built on feedback loops
Healthcare has spent decades trying to change people with education and motivation.
But behavior doesn’t change because someone was told what to do.
It changes when the right choice becomes obvious, measurable, and reinforced — day after day.
That’s what feedback loops make possible: a healthcare model where you don’t have to guess whether you’re getting healthier, and you don’t have to wait years to see the consequences of today’s decisions.
Because the point isn’t just living longer.
It’s getting more good years — more strength, more clarity, more freedom, more time fully present with the people you love.
Make outcomes visible. Reduce friction. Close the loop.
Give people their good years back.
Sources referenced
WHO (Adherence to Long-Term Therapies, 2003): https://iris.who.int/bitstream/handle/10665/42682/9241545992.pdf
National Academies — Best Care at Lower Cost (report brief): https://nap.nationalacademies.org/resource/13444/BestCareReportBrief.pdf
Lancet Digital Health umbrella review PDF (wearables): https://www.newswise.com/pdf_docs/165828208454252_PIIS258975002200111X.pdf
JCEM meta-analysis (CGM in T2D): https://academic.oup.com/jcem/article/109/4/1119/7438972
Feedback meta-analysis (physical activity): https://ijbnpa.biomedcentral.com/articles/10.1186/s12966-024-01635-5
NEHI report (wasteful/avoidable costs from suboptimal med use): https://www.nehi.net/wp-content/uploads/2019/07/Medication-Adherence-Appendix.pdf
HHS Telehealth Research Recap (RPM adoption): https://aspe.hhs.gov/sites/default/files/documents/0c3a38dcef21282e7d6c313b10799490/telehealth-rpm-research-recap.pdf
JAMA Network Open (cost-related nonadherence among older adults): https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2811037